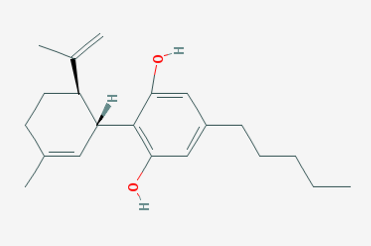
The emergence of high cannabidiol (CBD)-marijuana strains and CBD-rich medicinal products over the last 20 years has led to an explosion in the medicinal use of cannabis. CBD is an abundant non-psychoactive phytocannabinoid in cannabis that is thought to convey many of its medicinal benefits. While medicinal use of cannabis has been reported for centuries, it’s only recently been appreciated that CBD is responsible for many of its medicinal benefits. Pre-clinical and human clinical trials have demonstrated CBD’s ability to successfully treat a spectrum of disorders, lending credibility to amassing anecdotal reports . Importantly, CBD carries no addiction risk and has a low-side effect profile. This substantially enhances CBD’s medicinal utility and is helping CBD forge its way into modern medicine. Emerging evidence even identifies CBD as a tool to combat addiction and the opioid epidemic. These are exciting times for those seeking more efficacious and safe treatment options.
CBD has a high-safety profile
Until the late 90’s, CBD was largely disregarded by cultivators who sought to increase the concentration of Δ9-THC (i.e., the most abundant psychoactive phytocannabinoid) to meet the demands of recreational users looking to get stoned. A study of nearly 39,000 cannabis samples found that the average Δ9-THC potency jumped from 4% in 1995 to 12% in 20141. Four strains in the 2016 Cannabis Cup even topped the 30% Δ9-THC mark. People can now get higher than ever.
But with the increase in Δ9-THC potency, CBD levels in recreational strains have decreased to record lows. Since CBD can counteract Δ9-THC’s effects on brain function, the rapid escalation in the Δ9-THC:CBD ratio from 14 in 1995 to 80 in 2014 has led us to uncharted territory for understanding recreational cannabis’ acute and long-term safety profile.
Cannabis’ medicinal utility hinges on its safety profile, known as the therapeutic index (TI). The TI is the range between the effective dose (the dose used to treat a particular ailment) and the toxic dose (the dose that causes harm). Therefore, drugs that have a high TI are deemed “safe”. The TI for cannabis ranges depending on several factors including age of the user and chemical composition of the product/strain. The TI increases with age and a higher CBD: Δ9-THC ratio.
Δ9-THC exposure early in development is associated with numerous deleterious outcomes. Rodent studies have revealed that Δ9-THC is a developmental neurotoxin, and just a single exposure to Δ9-THC can induce long-term behavioral abnormalities2. Late adolescent exposure to Δ9-THC can also potentiate the development of schizophrenia-like symptoms in mice3. These animal studies support decades of human research showing that adolescent cannabis exposure increases risk of developing psychiatric illnesses including anxiety, depression and schizophrenia4.
Scientists are just beginning to reveal the cross-generational effects of Δ9-THC exposure. They are finding that your consumption of high- Δ9-THC strains doesn’t just affect you, but will affect your unborn children5. For instance, Δ9-THC exposure in adolescent rats increases addiction-like behavior in their offspring by altering genetic expression in the brain’s reward circuitry6. These studies highlight the relatively low-TI of Δ9-THC, especially in children and young adults.
In adults, Δ9-THC has a higher TI. Δ9-THC may be used to reduce nausea, provide pain relief, and as an appetite stimulant for patients on chemotherapy. But a single moderate dose of 10mg THC can induce anxiety and psychosis7, and long-term use is associated impaired executive function and memory8. So despite positive recreational effects of Δ9-THC, there is risk for adverse consequences.
CBD, on the other hand, has a higher TI in both children and adults. Several recent studies investigated CBD’s treatment potential in children with epilepsy and failed to detect significant side-effects9,10. While greater frequency of diarrhea, drowsiness, and fatigue was observed in the CBD-treated group, it’s important to note that these patients remained on their anti-epileptic medications for the extent of the trial. Because CBD is known to impact the metabolism of these other drugs, it’s unclear if CBD produced those side effects or if they resulted from an interaction with their additional medications.
CBD’s safety profile in adults has been more extensively tested, and these studies reveal a particularly high TI (summarized in 11). A single 600mg dose of CBD was not associated with any of the adverse effects of Δ9-THC described above7. In fact, even doses up to 1500mg/kg failed to induce significant adverse effects. For those seeking a long-term treatment strategy, chronic administration of 300mg CBD for over 4 months is well-tolerated and not associated with any toxic effects12.
Despite the increased side-effect risk of Δ9-THC consumption, many users still seek its medicinal benefits. Notably, CBD can increase Δ9-THC’s TI by counteracting its adverse effects. For instance, CBD reduces Δ9-THC’s anxiety-provoking effects in rodents13 and humans14,15, and strongly attenuates psychotic symptoms induced by Δ9-THC14,16. These studies reflect CBD impedance of Δ9-THC action at CB1 receptors, the target by which Δ9-THC exerts its psychoactive effects, either by reducing CB1 receptor activity17 or through direct antagonism18. Therefore, the addition of CBD to a Δ9-THC preparation reduces risk of adverse effects.
CBD treatment of neuropsychiatric disorders
Medicinal cannabis use has roots in ancient Chinese medical texts, in which writings discuss the use of hemp in medical practice and its use in “painless surgery”. The mention of hemp in ancient Chinese texts and lore suggests that CBD, which has higher potency in hemp than Δ9-THC, was responsible for many of the observed benefits associated with hemp. Today, we recognize the vast scope of CBD’s medicinal potential.
To date, there are 131 listed human clinical trials investigating CBD on various disorders (clinicaltrials.gov). For instance, studies are currently underway to assess CBD’s efficacy in treating autism, anxiety, schizophrenia, irritable bowel syndrome, over-eating, and opioid abuse (among many others). The broad scope of these CBD clinical trials highlights the escalating recognition that CBD has medicinal value in treating disorders that are otherwise poorly controlled by available medications. Furthermore, CBD’s low side-effect profile, as discussed above, makes CBD a promising therapeutic tool for treating these disorders and maintaining long-term compliance, especially in children. A subset of disorders in which CBD has positive medicinal indications are discussed below.
Epilepsy
Perhaps the most well-studied medicinal use of CBD is in treatment-resistant forms of epilepsy. According to the World Health Organization, there are 50 million people currently living with epilepsy, and 1 out of every 26 people will develop epilepsy in their lifetime. 20% of epilepsies cannot be controlled with traditional anti-epileptic medications. These “treatment-resistant” forms of epilepsy are usually caused by genetic mutations and seizures that begin in childhood and are often characterized by frequent seizures, and cognitive and behavioral deficits.
For reasons relating to cannabis’ Schedule I status under the Controlled Substance Act, cannabis, and particularly CBD, is not considered a first-line treatment. Children first exhaust an extensive regiment of anti-epileptic medications before their caregivers attempt cannabis. Only recently have physicians began to appreciate the anti-epileptic utility of cannabis. Recent clinical trials have revealed that twice daily oral doses of CBD (Epidolex, GW Pharmaceuticals), totaling 20mg/kg to 50mg/kg CBD, reduces seizure frequency in children with treatment-resistant epilepsies9,10. Children treated with CBD had a 39% median reduction in seizure frequency compared to 13% among the placebo-control group. Further, 62% of parents responded that CBD improved their child’s overall well-being compared to 35% in the placebo group10. CBD’s anti-epileptic effect, confirmed in these clinical trials, provide some relief for patients and their caregivers, but also legitimizes CBD’s use in the medical community.
Anxiety disorders
CBD is commonly used to treat anxiety. Pre-clinical studies in rats illustrate CBD’s ability to reduce anxiety in acutely stressful events. For example, rats given the option to explore an environment with both protected or exposed areas spend the majority of their time in the protected areas and sacrifice their desire to explore the exposed areas. CBD, however, increases the amount of time rats spend in the exposed areas19. This is a common example of a pre-clinical assessment that models anxiety-like behavior in humans, and consistently, CBD is found to reduce anxiety.
As an example in humans, those with generalized social anxiety disorder have difficulty interacting in daily life away from their home and engaging in public speaking. In a study of patients with social anxiety disorder, oral consumption of CBD (600mg, dissolved in corn oil) reduced anxiety, cognitive impairment, and overall discomfort associated with public speaking compared to a control group20. CBD’s anxiolytic effect on social anxiety illustrates its effectiveness in additional forms of anxiety including generalized anxiety disorder, obsessive-compulsive disorder, and post-traumatic stress disorder21 (note: PTSD and OCD are no longer classified as anxiety disorders in the recent DSM-V, but excessive anxiety underlies symptoms of these disorders).
Importantly, CBD’s anxiolytic effects follow an inverted-U response19, in which there’s an optimal dose range for treating anxiety. CBD doses above this range lose their anxiolytic quality. So when using CBD to treat anxiety, if it initially fails to have an effect, the best strategy would be to first reduce the CBD dose. If after that point it is still ineffective, then try a higher dose.
Psychosis
Heavy cannabis use during adolescence is a risk factor for developing schizophrenia4. However in adulthood, CBD may be the best treatment22. While positive symptoms in schizophrenia (e.g., hallucinations, delusions) are usually responsive to traditional antipsychotic medications, negative symptoms (e.g., apathy, low affect, impaired cognition) are more difficult to treat. In one clinical trial comparing the effect of oral CBD (600mg/day) to amisulpride, a traditional antipsychotic, both drugs improved negative symptoms, but CBD (3x daily 200mg CBD capsules) had a superior side-effect profile than amisulpride23. CBD has also been demonstrated to enhance the ability of antipsychotic medication to reduce positive symptoms when used as an adjunctive therapy, and there’s evidence from case studies that CBD effectively reduces symptoms in treatment-resistant forms of schizophrenia24.
Psychosis is also common in Parkinson’s disease. A small open-label clinical trial found that CBD reduced psychosis without negatively impacting the disease’s motor impairments25. A subsequent investigation found that CBD, in oral capsules of 300mg/day but not 75mg/day, increased the quality of life in Parkinson’s patients. It’s unclear, however, if this is due to a reduction in psychotic symptoms or through CBD’s anxiolytic/antidepressant effects26. Together, these results highlight CBD’s potential as an effective treatment of psychosis with a lower side-effect profile than traditional antipsychotic medications.
The wide range of CBD’s medicinal effects reflects its multiple brain and body targets27. CBD’s antiepileptic, anxiolytic, and antipsychotic effects may stem from its ability to enhance inhibitory GABAergic signaling and serotonergic signaling. These neural mechanisms are similar to the actions of benzodiazepines and selective serotonin reuptake inhibitors (SSRIs), respectively, which are commonly prescribed pharmacological treatment for anxiety, depression, and epilepsy. CBD’s enhancement of the brain’s endogenous cannabinoid, 2-AG23, and partial agonism of dopamine D2 receptors28, the target of antipsychotic medications, likely contribute to its antipsychotic effects.
Pain
CBD has long been known for its analgesic and anti-inflammatory action29. Compared to the abundant phytocannabinoids Δ9-THC and cannabinol, CBD is the most effective at reducing peripherally-induced pain and inflammation30. There’s evidence for CBD’s analgesic (i.e., pain-reducing) effects on both inflammation-induced pain and neuropathic pain. For instance, arthritis is a form of chronic inflammatory-derived pain that affects over 20% of Americans older than 18. Arthritis-like pain can be created in the laboratory with exposure to a topical solution known as Freund’s adjuvant which enhances local inflammation and induces pain. Researchers found that topical CBD gel (i.e., applied to the skin) reduces pain by inhibiting the inflammation and swelling induced by Freund’s adjuvant31. In addition to topical CBD, oral consumption of CBD (2.5-20mg/kg) has also been shown to reduce inflammatory pain caused by Freund’s adjuvant32. There are therefore multiple administration routes by which CBD can reduce inflammation-derived pain.
CBD also has promise for treating neuropathic pain, which may be caused by a host of factors including nerve constriction, diabetes, and chemotherapy. In rats, CBD (20mg/kg) reduced pain caused by sciatica32, a form of neuropathic pain resulting from constriction of the sciatic nerve that causes radiating pain down the legs and back. Neuropathic pain caused by chemotherapy drugs is a common challenge in cancer treatment that further diminishes quality of life for cancer patients. Intriguingly, CBD (10-20mg/kg) reduced chronic pain caused by chemotherapy drugs in mice33,34. Further, the combination of CBD and the chemotherapy drug, Paclitaxel, reduced the viability of breast cancer tumor cells more than either drug alone34. These studies highlight CBD’s analgesic qualities in addition to its anticancer effects35,36.
Emerging potential for CBD in combating opioid addiction
The scope of CBD’s treatment potential is vast. Because of its low side-effect profile, CBD may be the optimal therapeutic strategy for many patients regardless if they’re on traditional medications or are trying to combat treatment-resistant disorders. Still, an increasing number of potentially promising CBD indications are being revealed. One promising future direction is its ability to combat opioid addiction.
The current opioid epidemic is killing us. Of the 55,000 lethal drug overdoses each year, 33,000 are from opioids. 20,000 of these overdoses result from prescription opioids, and most of the remaining are from heroin. Over 60% of these lethal overdoses are deemed “accidental”, highlighting the loss-of-control associated with opioid use. One of the best tools to combat the opioid epidemic may be cannabis and CBD.
Addiction is characterized not just by intoxication from drug use, but long-lasting disturbances in cognitive performance and emotional states that lead to craving and relapse. Thus, reducing craving and propensity for relapse would substantially aid an addict’s ability to overcome addiction. Anxiety is enhanced in addiction and peaked during periods of withdrawal, leading to further drug taking and relapse. Reducing anxiety in addiction would be a powerful step in curbing drug seeking. Fortunately, one of the most consistent and reproducible effects of CBD is its ability to reduce anxiety21, thus highlighting its potential to reduce risk of drug relapse.
Indeed, there’s evidence from pre-clinical studies that CBD can reduce the risk of heroin relapse. In one study37, rats were trained to press a lever for heroin. The rats learned that they would receive an IV infusion of heroin (via an implanted catheter) only when they pressed the lever in the presence of a cage light. In this case, the cage light served as a cue for heroin availability. As you can imagine, when the light was on, they’d press away. It’s similar to an addict approaching an alley where they’re used to shooting up, and if a light is on above the door, they know that someone has heroin inside. When the light is on, they approach the door and receive heroin.
Two weeks later, the researchers put the rats back in the same chamber in which they received heroin. When the light would turn on, the rats would, again, press away to receive heroin. One group of rats, however, received CBD (5mg/kg) the day before being placed back in the chamber. When the light went on, the rats that received CBD made far fewer lever press attempts to get heroin than those in the control group. It’s as if a heroin user who consumed CBD would be more likely to pass by the alleyway without getting heroin, even if the light was on above the door. The authors conclude that this reduction in cue-induced heroin seeking stemmed from CBD’s ability to normalize changes in the brain’s reward circuitry that result from repeated heroin use. This study suggests that CBD may protect against opioid relapse following a period of abstinence.
Another recent report found that CBD (10mg/kg) reduced the conditioned place preference for morphine in mice38. To conceptualize the significance of this finding, imagine coming out of surgery and being given morphine to combat the pain. Not only does the morphine combat the pain, but it activates the brain’s reward center. Over time you crave the morphine, both for its pain-relieving effects and the pleasure it induces. You eventually leave the hospital but continue to crave the opioid kick. Instead of morphine, you take prescription pain meds like Oxycontin or Percocet. The pain from the surgery should have largely subsided, but you feel crummy if you don’t take your pain meds. So you seek more. Maybe your doctor prescribes another round, maybe they don’t. It turns out that heroin is cheaper, and stronger anyway. As tolerance to the drugs sets in, you find yourself needing to take increasing amounts of the pain medications just to feel normal. With increased consumption, your risk of overdose increases, especially as you seek stronger drugs and new environments to consume them.
Now imagine that instead of receiving just morphine in the hospital after your surgery, you received morphine in addition to CBD. What the pre-clinical studies suggest is that the combination of two will make you less motivated to seek opioids once you leave the hospital because you didn’t find its use as rewarding as if you would have taken morphine alone (note: because of morphine’s Schedule II status under the Controlled Substance Act, it’s logistically easier and more accessible to study than heroin or cannabis. Because of morphine’s similarity to heroin, it’s effects are often generalized to most opioid drugs). Since CBD alone also has pain-relieving effects, the combination can also have synergistic effects to strongly reduce pain39 while reducing the drive to continue future opioid use.
Concluding remarks
While many of CBD’s medicinal benefits are well-accepted in the cannabis community, there is still skepticism among the medical professionals. The accumulation of positive clinical trials is helping, but progress remains sluggish. CBD and other cannabinoids are rarely considered first-line treatment options, in part due to the relative dearth of clinical evidence. This reflects the research burdens imposed by cannabis’ Schedule I status, which makes it excessively burdensome to conduct cannabis research (and yes, that includes CBD-only research). By definition, a Schedule I drug has no medicinal benefit. This makes it especially challenging to convince a funding agency to award money to study the medicinal value of CBD. However, the tides may be turning. In 2015 the National Institute of Health allotted $21.2 million towards medicinal cannabis research. As more research funding is allocated towards pre-clinical and clinical trials of CBD and other cannabinoids, a more comprehensive understanding of their medicinal value will be recognized and appreciated. Slowly, CBD may be included in routine clinical practice, but this will likely require the removal of cannabis’ Schedule I status. Until the shift in public policy (and federal law), many patients who are unaware of CBD’s medicinal utility, or do not have access, may unfortunately sacrifice their most efficacious and safe treatment option. But for those in-the-know, your local dispensary may be the optimal pharmacy.
1 ElSohly, M. A. et al. Changes in Cannabis Potency Over the Last 2 Decades (1995-2014): Analysis of Current Data in the United States. Biol Psychiatry 79, 613-619, doi:10.1016/j.biopsych.2016.01.004 (2016).
2 Philippot, G., Nyberg, F., Gordh, T., Fredriksson, A. & Viberg, H. Short-term exposure and long-term consequences of neonatal exposure to Delta(9)-tetrahydrocannabinol (THC) and ibuprofen in mice. Behav Brain Res 307, 137-144, doi:10.1016/j.bbr.2016.04.001 (2016).
3 Rodriguez, G. et al. Delta9-tetrahydrocannabinol (Delta9-THC) administration after neonatal exposure to phencyclidine potentiates schizophrenia-related behavioral phenotypes in mice. Pharmacol Biochem Behav 159, 6-11, doi:10.1016/j.pbb.2017.06.010 (2017).
4 Chadwick, B., Miller, M. L. & Hurd, Y. L. Cannabis Use during Adolescent Development: Susceptibility to Psychiatric Illness. Front Psychiatry 4, 129, doi:10.3389/fpsyt.2013.00129 (2013).
5 Szutorisz, H., Egervari, G., Sperry, J., Carter, J. M. & Hurd, Y. L. Cross-generational THC exposure alters the developmental sensitivity of ventral and dorsal striatal gene expression in male and female offspring. Neurotoxicol Teratol 58, 107-114, doi:10.1016/j.ntt.2016.05.005 (2016).
6 Szutorisz, H. et al. Parental THC exposure leads to compulsive heroin-seeking and altered striatal synaptic plasticity in the subsequent generation. Neuropsychopharmacology 39, 1315-1323, doi:10.1038/npp.2013.352 (2014).
7 Martin-Santos, R. et al. Acute Effects of a Single, Oral dose of d9-tetrahydrocannabinol (THC) and Cannabidiol (CBD) Administration in Healthy Volunteers. Current Pharmaceutical Design 18, 4966-4979, doi:10.2174/138161212802884780 (2012).
8 Crean, R. D., Crane, N. A. & Mason, B. J. An evidence based review of acute and long-term effects of cannabis use on executive cognitive functions. J Addict Med 5, 1-8, doi:10.1097/ADM.0b013e31820c23fa (2011).
9 Devinsky, O. et al. Cannabidiol in patients with treatment-resistant epilepsy: an open-label interventional trial. The Lancet Neurology 15, 270-278, doi:10.1016/s1474-4422(15)00379-8 (2016).
10 Devinsky, O. et al. Trial of Cannabidiol for Drug-Resistant Seizures in the Dravet Syndrome. N Engl J Med 376, 2011-2020, doi:10.1056/NEJMoa1611618 (2017).
11 Bergamaschi, M. M., Queiroz, R.H.C., Crippa, J.A.S., & Zuardi, A.W. Safety and Side Effects of Cannabidiol, a Cannabis Sativa Constitent Curr Drug Saf 6, 237-249 (2011).
12 Cunha, J. M. et al. Chronic Administration of Cannabidiol to Healthy Volunteers and Epileptic Patients. Pharmacology 21, 175-185, doi:10.1159/000137430 (1980).
13 Todd, S. M. & Arnold, J. C. Neural correlates of interactions between cannabidiol and Delta(9) -tetrahydrocannabinol in mice: implications for medical cannabis. Br J Pharmacol 173, 53-65, doi:10.1111/bph.13333 (2016).
14 Morgan, C. J. et al. Sub-chronic impact of cannabinoids in street cannabis on cognition, psychotic-like symptoms and psychological well-being. Psychol Med 42, 391-400, doi:10.1017/S0033291711001322 (2012).
15 Zuardi, A. W., Shirakawa, I., Finkelfarb, E., & Karniol, I.G. Action of cannabidiol on the anxiety and other effects produced by delta-9-THC in normal subjects. Psychopharmacology 76, 245-250 (1982).
16 Bhattacharyya, S. et al. Opposite effects of delta-9-tetrahydrocannabinol and cannabidiol on human brain function and psychopathology. Neuropsychopharmacology 35, 764-774, doi:10.1038/npp.2009.184 (2010).
17 Laprairie, R. B., Bagher, A. M., Kelly, M. E. & Denovan-Wright, E. M. Cannabidiol is a negative allosteric modulator of the cannabinoid CB1 receptor. Br J Pharmacol 172, 4790-4805, doi:10.1111/bph.13250 (2015).
18 Thomas, A. et al. Cannabidiol displays unexpectedly high potency as an antagonist of CB1 and CB2 receptor agonists in vitro. Br J Pharmacol 150, 613-623, doi:10.1038/sj.bjp.0707133 (2007).
19 Guimarães, F. S., Chiaretti, T. M., Graeff, F. G. & Zuardi, A. W. Antianxiety effect of cannabidiol in the elevated plus-maze. Psychopharmacology 100, 558-559, doi:10.1007/bf02244012 (1990).
20 Bergamaschi, M. M. et al. Cannabidiol reduces the anxiety induced by simulated public speaking in treatment-naive social phobia patients. Neuropsychopharmacology 36, 1219-1226, doi:10.1038/npp.2011.6 (2011).
21 Blessing, E. M., Steenkamp, M.M., Manzanares, J., & Marmar, C.R. Cannabidiol as a potential treatment for anxiety disorders. Neurotherapeutics 12, 825-836, doi:10.1007/s13311-015-0387-1 (2015).
22 Ruggiero, R. N. et al. Cannabinoids and Vanilloids in Schizophrenia: Neurophysiological Evidence and Directions for Basic Research. Front Pharmacol 8, 399, doi:10.3389/fphar.2017.00399 (2017).
23 Leweke, F. M. et al. Cannabidiol enhances anandamide signaling and alleviates psychotic symptoms of schizophrenia. Transl Psychiatry 2, e94, doi:10.1038/tp.2012.15 (2012).
24 Fasinu, P. S., Phillips, S., ElSohly, M. A. & Walker, L. A. Current Status and Prospects for Cannabidiol Preparations as New Therapeutic Agents. Pharmacotherapy 36, 781-796, doi:10.1002/phar.1780 (2016).
25 Zuardi, A. W., Crippa, J.A.S., Hallak, J.E.C., Pinto, J.P., Chagas, M.H.N, Rodrigues, G.G.R., Dursun, S.M., & Tumas, V. Cannabidiol for the treatment of psychosis in Parkinson’s disease Journal of Psychopharmacology 23, 979-983 (2009).
26 Chagas, M. H. et al. Effects of cannabidiol in the treatment of patients with Parkinson’s disease: an exploratory double-blind trial. J Psychopharmacol 28, 1088-1098, doi:10.1177/0269881114550355 (2014).
27 Pertwee, R. G. The diverse CB1 and CB2 receptor pharmacology of three plant cannabinoids: delta9-tetrahydrocannabinol, cannabidiol and delta9-tetrahydrocannabivarin. Br J Pharmacol 153, 199-215, doi:10.1038/sj.bjp.0707442 (2008).
28 Seeman, P. Cannabidiol is a partial agonist at dopamine D2High receptors, predicting its antipsychotic clinical dose. Transl Psychiatry 6, e920, doi:10.1038/tp.2016.195 (2016).
29 Brand, E. J. & Zhao, Z. Cannabis in Chinese Medicine: Are Some Traditional Indications Referenced in Ancient Literature Related to Cannabinoids? Front Pharmacol 8, 108, doi:10.3389/fphar.2017.00108 (2017).
30 Formukong, E. A., Evans, A.T., & Evans, F.J. Analgesic and antiinflammatory activity of constituents of Cannabis sativa L. Inflammation 12, 361-371 (1988).
31 Hammell, D. C. et al. Transdermal cannabidiol reduces inflammation and pain-related behaviours in a rat model of arthritis. Eur J Pain 20, 936-948, doi:10.1002/ejp.818 (2016).
32 Costa, B., Trovato, A. E., Comelli, F., Giagnoni, G. & Colleoni, M. The non-psychoactive cannabis constituent cannabidiol is an orally effective therapeutic agent in rat chronic inflammatory and neuropathic pain. Eur J Pharmacol 556, 75-83, doi:10.1016/j.ejphar.2006.11.006 (2007).
33 King, K. M. et al. Single and combined effects of Delta9 -tetrahydrocannabinol and cannabidiol in a mouse model of chemotherapy-induced neuropathic pain. Br J Pharmacol 174, 2832-2841, doi:10.1111/bph.13887 (2017).
34 Ward, S. J. et al. Cannabidiol inhibits paclitaxel-induced neuropathic pain through 5-HT(1A) receptors without diminishing nervous system function or chemotherapy efficacy. Br J Pharmacol 171, 636-645, doi:10.1111/bph.12439 (2014).
35 Sarfaraz, S., Adhami, V. M., Syed, D. N., Afaq, F. & Mukhtar, H. Cannabinoids for cancer treatment: progress and promise. Cancer Res 68, 339-342, doi:10.1158/0008-5472.CAN-07-2785 (2008).
36 Elbaz, M. et al. Modulation of the tumor microenvironment and inhibition of EGF/EGFR pathway: novel anti-tumor mechanisms of Cannabidiol in breast cancer. Mol Oncol 9, 906-919, doi:10.1016/j.molonc.2014.12.010 (2015).
37 Ren, Y., Whittard, J., Higuera-Matas, A., Morris, C. V. & Hurd, Y. L. Cannabidiol, a nonpsychotropic component of cannabis, inhibits cue-induced heroin seeking and normalizes discrete mesolimbic neuronal disturbances. J Neurosci 29, 14764-14769, doi:10.1523/JNEUROSCI.4291-09.2009 (2009).
38 Markos, J. R., Harris, H. M., Gul, W., ElSohly, M. A. & Sufka, K. J. Effects of Cannabidiol on Morphine Conditioned Place Preference in Mice. Planta Med, doi:10.1055/s-0043-117838 (2017).
39 Neelakantan, H. et al. Distinct interactions of cannabidiol and morphine in three nociceptive behavioral models in mice. Behav Pharmacol 26, 304-314, doi:10.1097/FBP.0000000000000119 (2015).